What is needed is better public health communication.
Sarojini Nadimpally
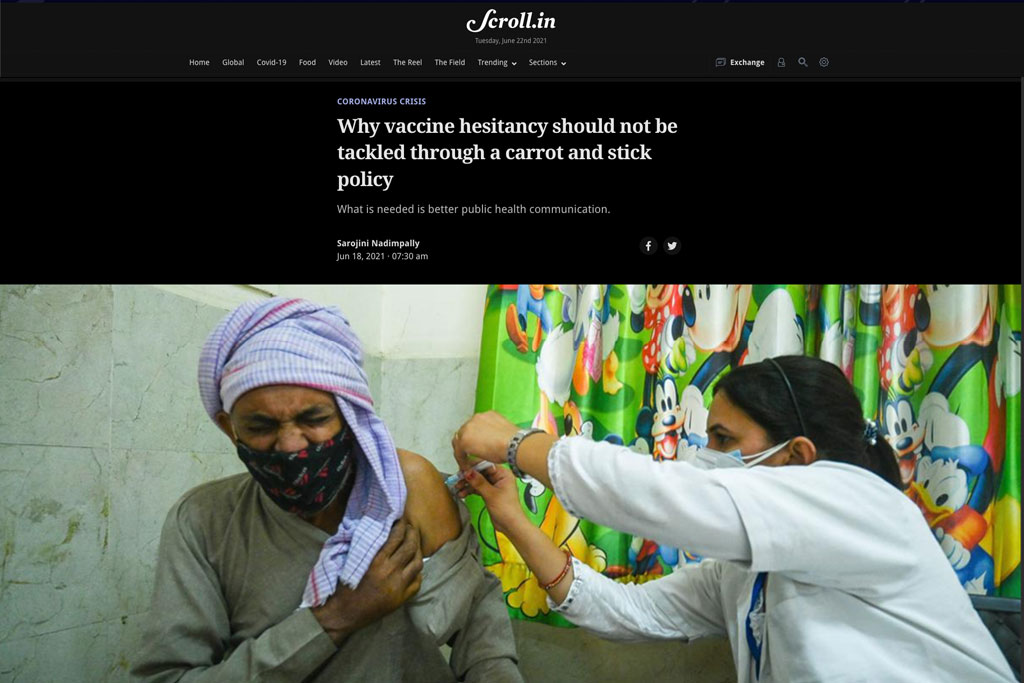
Along with an acute shortage of Covid-19 vaccines, with only 3.3% of its population fully vaccinated, India is also witnessing vaccine hesitancy. Anecdotal evidence suggests people, particularly in the rural and tribal areas, are not coming forward to take the vaccines. While it is imperative to address vaccine hesitancy, superficial attempts that fail to understand its structural causes could lead to more damage.
As an organisation working on health access in different parts of the country, we have found several rumors and misplaced perceptions are circulating on the ground. In rural Maharashtra, Chhattisgarh, Odisha, Madhya Pradesh, Rajasthan and Uttar Pradesh, many people are hesitant because they have heard about deaths within 15 -20 days of getting the vaccine.
Rani, who works with an NGO in Jharkhand, came across a rumour that Covid-19 vaccines lead to infertility. When she enquired about the source of this information from the person who had shared it with her, he said: “Aisa sunne mein aaya tha. That’s what we’ve heard.” Another frontline worker in Chhattisgarh said people in her area were hesitant to get vaccinated as they believe the vaccines can cause Covid symptoms and complications, even death.
Social media and messaging platforms are also filled with unverified claims and rumours about vaccines. In April, a message titled “A reminder for all women,” went viral. It claimed that adolescent girls need to be cautious about getting vaccinated. “Don’t take the vaccine before and after 5 days of your periods because immunity will be very less during periods,” it said, falsely claiming that there was a “high risk of attack for one who vaccinated during periods”.
What has added to the skepticism in some quarters is the way clinical trials were conducted at warp speed, the questionable basis for emergency authorisation approvals, the uncertainty about possible adverse effects, and the lack of a robust mechanism to address them. Many public health advocates have been repeatedly raising issues about the lack of transparency of information at every stage of vaccine development. Further, the lack of involvement of the community and civil society in vaccine policy has seriously impaired trust, which has probably influenced the negativity of people towards vaccination.
It must be acknowledged that vaccine hesitancy does not arise out of the thin air overnight. These rumours, myths, and perceptions aiding hesitancy prevail in the absence of credible and accessible information. The need for public health messaging is all more crucial to enable the marginalised to make informed decisions about vaccination. In absence of trusted sources of information, the vaccine uptake is inevitably impacted.
To believe that the government could handle this with an over-emphasis on a “digital solution” is far too misplaced as it only makes a mockery of India’s digital divide.
Disincentives and incentives
Instead of addressing the root causes of vaccine hesitancy, local authorities across states are resorting to veiled as well as open threats in the rural areas.
In Pratapgarh, Uttar Pradesh, people reportedly have been threatened that their ration and MGNREGA wages will be withheld if they don’t take the vaccine. In Bulandshahr, the police have been making public announcements that businessmen 45 years and above will not be allowed to run their shops and business establishments without vaccination.
An administrator in Rajasthan reportedly threatened to not give food ration to those who did not get vaccinated. Even the Indian Medical Association has recommended: “Vaccination certificate shall be made a mandatory certificate for entering into public places and receiving products under the public distribution system.”
The flip side of disincentives are incentives. A Chennai-based Foundation is providing lucky draws with prizes such as gold coins, washing machines, blenders and bikes to those who take the vaccines. The Sheohar district administration in Bihar is reported to be adopting this model to overcome vaccine hesitancy. News reports said the goldsmith community in Rajkot, Gujarat, had provided freebies to encourage more people for vaccination in April.
A recent appeal to the Prime Minister by the Jan Swasthya Abhiyan, Rajasthan chapter, proposes families that are fully vaccinated be given 150 days of MGNREGA work instead of the regular 100 days and 7 Kg of grain per person per month instead of 5 kg. It also recommends that all pregnant and lactating mothers be given one free hot cooked meal post two shots of vaccination.
An older debate
The debates on incentives and disincentives have a long history, particularly in the women’s rights and health rights movements that have critiqued incentivised, target driven sterilisation.
Many health researchers argue that making health insurance to a family living below the poverty line conditional on sterilisation may appear on the surface to be an important incentive, but it shifts the onus of health care access on to the marginalised – if they are denied insurance it is because they were not willing to get sterilised.
In the past, health advocates were concerned about the Tamil Nadu government’s decision to make disbursal of the third instalment of the Mutthu Lakshmi Reddy Maternity Benefit Scheme in Tamil Nadu dependent on completion of all three pentavalent vaccines by 14 weeks and measles vaccine at nine months.
The incentives outlined in JSA Rajasthan’s appeal including the one hot cooked meal for pregnant women, shifts the burden on to communities without enhancing government accountability in any way. This is deeply problematic as the Covid-19 pandemic and the lockdowns have exacerbated already existing inequities, with marginalised communities having reduced economic opportunities, lack of access to health facilities, food and nutrition.
Further linking employment availability and food rations to acceptance of vaccination is unacceptable from an equity, rights and social justice perspective.
Equity and access to vaccination
Vaccine hesitancy is deeply embedded in the breakdown of trust in the health system, based on past experiences of people. Lack of informational transparency heightens concerns about post vaccination effects disrupting work rhythms.
To address vaccine hesitancy, it is extremely important to understand the regional and cultural practices of the communities; their health-seeking behaviors, experiences, fears; mobility and access challenges; capacity to navigate through the digital divide; as well as take the effort to reach authentic and trusted health information to the people.
It is the responsibility of the state to dispel myths, answer concerns and queries, and offer information in a timely and accessible manner. We need to ask the government what steps have been taken to address the vaccine hesitancy directly and whether these initiatives and efforts are adequate and just.
This must be accompanied by reliable information on the available vaccines accompanied with vaccine availability, regulatory issues related to transparency around approvals and licensing, and monitoring adverse effects post immunisation, needless to say in languages and forms that are easily assimilated by people.
Incentives and disincentives cannot compensate for these gaping holes in information dissemination and solve the larger structural inequities. An effort should be made to work around this problem through coordinated efforts between the government and civil society, community leaders, frontline workers and health care providers and media. That depends on how effectively the country invests in its people, giving them better facilities in spheres of general health, education, political and economic opportunities.
Sarojini Nadimpally is public health practitioner associated with Jan Swasthya Abhiyan (National) and Sama Resource Group for Women and Health.
The author acknowledges Deepa, Sweta, Aakriti and Neelanjana for their support.
This article was carried on Scroll.In on 18 June 2021. Read original article.



